How to Treat Spondylolisthesis in Dancers
Dear Lisa,
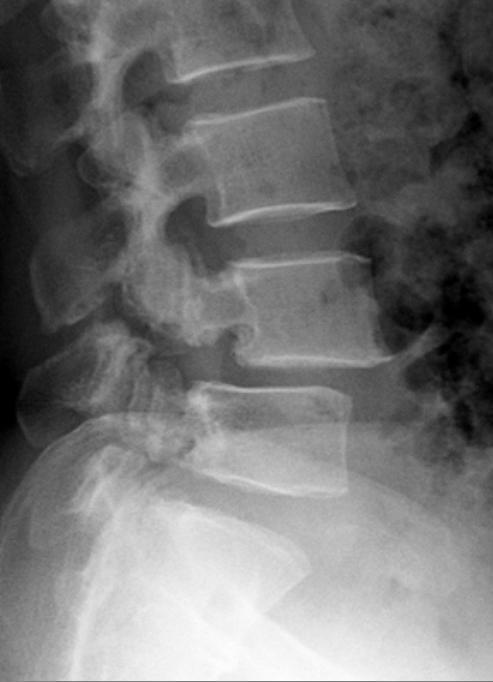
A friend of mine recommended I contact you as my 12 year old daughter has been diagnosed with a Bilateral Pars Defect with a minor Spondylolisthesis of L5.
She is a classical ballet dancer, and although she is not training full-time, she currently does approximately 16hrs/week of classes and also approximately 1 hour of stretching/strengthening at home each day. After a prolonged period of lower back pain which did not seem to ease (despite receiving physio treatments) and actually intensified during arabesques and extension movements she was sent for an X-Ray and Bone Scan approximately 3 weeks ago, which confirmed the diagnosis.
I have since been reading a great deal about this condition. My daughter is currently seeing a general physio, and also a physio who specialises in treating dancers. There seems to be a fair amount of conflicting information regarding a treatment plan for Pars fractures in dancers. I was hoping you may be able to offer me some advice on how to treat Spondylolisthesis in dancers.
Would you recommend absolute rest from all activities including core-strengthening pilates for a certain amount of time or would you recommend commencing a core programme immediately? Do you suggest 3-6 months as a recovery period?
She is only walking for exercise at present and is also doing a very stationary core programme. One of the physios recommended a core program on a Core Fitness Roller, to start immediately. The other dance physio used an ultra sound machine to determine which core muscles she switches on when she is dancing or doing abdominal work. Unfortunately she has been using the incorrect, bigger abdominal muscles instead of the smaller, deeper, intrinsic muscles. This physio has said no to a CFR programme until she can find and engage the right muscles.
I am inclined to agree with this, but I am not sure what she should or shouldn't be doing. I have read about 3 month treatment plans on the internet but I don't know if this is the norm.
Then there is the question of "to brace or not to brace?". I am so confused. I was hoping you may have treated dancers with this condition and could possibly offer me some advice for my daughter please. I am most grateful for your time. Thank you in advance.
Regards A.
Hi A
Thank you so much for your email, and please do not worry. While this is a tough injury to work with, I do have a student who had the exact same injury who is now dancing professionally overseas, so if dealt with correctly then she should be able to recover. You are correct in the fact that there is not much information on how to treat Spondylolisthesis in dancers.
Far too often the weakness in the lumbar spine that leads to this kind of injury have occurred due to excessive training into extension. This may not have necessarily happened in class, but unfortunately due to the extreme positions documented in so many photos and videos on social media these days, students often try to push themselves into some very unsafe positions. Had she been trying to work on back extensions, back scorpions etc at home in her stretching regime? It is essential in any rehab program to determine the cause of the injury, so if this was a factor, then she will need to go through ALL of the stretches that she was doing before the injury with her physio to determine their level of safety, and most probably, to revise her ongoing program to help her continue to improve in a much safer way.

I definitely agree with the second physio on this one. It is essential that she learn to correctly activate not only her deep abdominals and pelvic floor, but the Multifidus and other segmental stabilisers of the spine, ideally by using the visual ultrasound. If she attempts the higher level core program on the foam roller, but is using the wrong muscles, she will simply be training the wrong muscles. Dancers are FANTASTIC at cheating and she will probably be able to ‘do’ all of the exercises on the foam roller by bracing with her outer abdominals.
3 months is a good timeline to build back into dancing, and it must be taken very slowly.
The decision to brace must be made by the treating specialist, however I advise that even if she is braced, the core training with the ultrasound is essential and should be the core component of her rehab in the early stages. She should also be focussing on maintaining strength and control in her turnout, pelvic stability, and foot and ankle control. One of the biggest issues in dancers is losing condition in other parts of their body while they are rehabilitating another area. This is why we developed the “Will I Ever Dance Again?” program for foot injuries, and a modified version of this program, as guided by her therapist, can be used to make sure that she returns to dance at full strength.
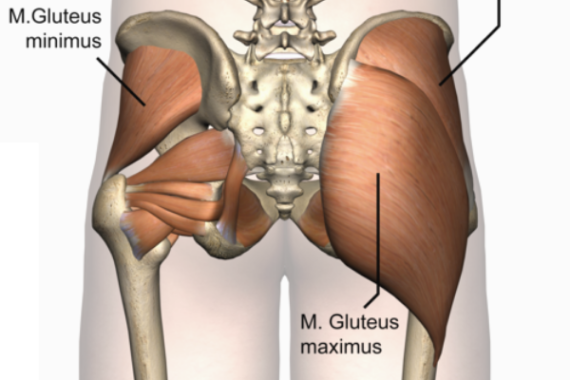
Two big areas of focus that must be achieved (in addition to the stabilisation of the spine) are improving her range of hip extension and Thoracic (upper back) extension. Learning how to use these two areas effectively can massively reduce the load that is placed through the lumbar spine. Arabesques and Extensions are the positions that will aggravate a Spondylolisthesis as initially (in so many students) most of the load is taken through the low back. However, with careful training, specific releases, and stretches to these areas, she should slowly be able to take the leg into extension again.
Obviously, this all depends on the magnitude of the Spondylolisthesis and will need to be discussed with the treating specialist, but I hope this helps!
Kindest Regards,
Lisa

P.S - Since publishing this post I have had requests for more detail on specifics of the rehab program I use with this injury. Unfortunately, I can't provide much more detail online. With a condition such as this, I highly advise that each individual's rehab program is individually customised as per their particular restrictions. For example, the program for a 65-year-old ex-professional dancer or teacher would be very different than the one for the 12-year-old dancer in the post! I have mentioned as much as I can, without the risk of people trying to treat themselves. In all cases, there must be a focus on improving mobility and extension of the upper back, and true hip extension, as well as guided stabilisation of the low back using the Visual Ultrasound. The program must be constantly reviewed and refined as you progress, so it is impossible for me to articulate this all in one post! I do go through the rehab of this in more detail in my 3 day intensive teachers course, which is the more appropriate platform to discuss this kind of high-level rehab.
I hope this helps and wish you all the best with your rehab.
Injury Resources
If you are looking to delve deeper into this topic, check out the following programs:
- Will I Ever Dance Again: The “Will I Ever Dance Again?” program is perfect if you are unable to train at full capacity, whether this is due to a foot injury, surgery, an accident or illness outside of the studio. It helps you build back to full capacity gradually, while maintaining strength, flexibility and control in the rest of the body.
- Level One Dance Teacher and Therapist Training: This unique course covers a multitude of assessment and treatment techniques to individualise a dancer's training. With special focuses on Postural Control, Core Stability, Flexibility, Basic Classical Technique, The Dancers Hip, Allegro, Spinal Mobility and Arabesques, it is suitable for anyone working closely with dancers.